Precancerous diseases of the vulva, vagina, cervix
- font size decrease font size increase font size
Precancerous diseases are conditions that tend to become malignant but do not necessarily do so (conditions with a malignant predisposition).Epithelial precancers may be
1. Glandular–eg, adenomatous hyperplasia–endometrium and adenomatous polyps
2. Squamous–eg, dysplasia of the uterine cervix or other urogenital mucosae.
The concept of "precancer" is a good explanation of the theory of carcinogenesis, according to which precancer is one of the phases in the overall process of carcinogenesis.
The first phase of this process - diffuse abnormal hyperplasia, the second - the formation of focal proliferations, and the third - the appearance of benign tumors and the fourth - the development of malignant tumors. The second and third phases, according to this theory, are actually precancer (obligate form), the first - represents an unfavorable background for the development of malignant tumor, precancer and cancer (optional form).
The basis for the diagnosis of precancer is morphological changes in the various reproductive organs.
Pre cancer of external genitaliaconsist of two stages: background diseases and pre malignant conditions.
The precancerous lesions of the external genitalia includes kraurosis and leukoplakia. These chronic degenerative processes of the mucocutaneous tissues and subcutaneous adipose tissue occur predominantly in the pre-and postmenopausal women and rarely at a young age. They make up 0,06% of the total number of gynecological diseases
Kraurosis vulvae An atrophic disease affecting the female external genitalia, most often of older women, resulting in drying and shriveling of the parts, and marked by leukoplakic patches on the mucosa, itching, dyspareunia, dysuria, and soreness, often accompanied by a chronic inflammatory reaction in the deeper tissues. It occurs most commonly as a result of lichen sclerosus et atrophicus of the vulva, but may be associated with other types of genital atrophy. It is also known as Vulva Lichen Sclerosus/ Breisky disease.
There are three stages of the disease:
I.Edematous - is characterized by edema, hyperemia of the external genitalia. The skin becomes tense, shiny, has a color from normal to bright red with a bluish tint. Large and small genital lips look swollen, hypertrophic.
II.In stage II has progressed markedly atrophic changes, flattened, large and small labia, clitoral atrophy occurs, the skin becomes inelastic, dry, whitish color, a kind of "polished", the vaginal opening narrows.
III.Stage III - fibrosclerotic - leads to complete atrophy and sclerosis of the external genitalia. Labia majora are transformed into thin, flat ridges, small - shrivel, becoming barely noticeable or completely disappear, decreasing the clitoris. In connection with the disappearance of hair follicles in the labia lips, no hair, sharply reduced the number of sebaceous glands. Skin and mucous thinner, becoming dull pearl color with gray-blue hue. As a result, multiple sclerosis, loss of elastic tissue in the vulva is easily assembled and folds looks like crumpled parchment sheet with a dull sheen. Sclerosis tissue causes a narrowing of the entrance of the vagina, the narrowing of the external opening of urethra and anus. Sexual intercourse is difficult or even impossible, can be difficult and painful urination. Narrowing the entrance to the vagina should be considered in the inspection of the cervix with the help of mirrors (for the inspection should take only small mirrors, pre-brushing them with petroleum jelly).
Leukoplakia is a condition that causes the growth of thick, white patches (known as plaques) to develop on the mucous membranes external genitalia (it describes patches of keratosis).
In the surface epithelium is revealed hyperkeratosis, parakeratosis, acanthosis. Further develops sclerosis tissues.
Combination kraurosis and leukoplakia is unfavorable for malignancy, especially in those parts of the vulva, where there is leukoplakia.
There are three degrees of hyperkeratosis:
·a flat,
·hypertrophic
·and warty.
Leukoplakia in the form of dry white or bluish-white plaques may be placed in limited areas or spread to the entire vulva. There are also contour and diffuse forms of leukoplakia.
Etiology and pathogenesis.
The basis of kraurosis and leukoplakia are complex neuroendocrine and metabolic disorders resulting from age-related functional changes in the higher divisions of the CNS, increased excitability of the hypothalamic structures involved in the regulation of gonadotrophic pituitary function, and centers related to the manifestation of vegetative nervous system actions. These patients often display decreases in the function of the adrenal cortex, decreases in the amount of corticosteroids in the tissues of the vulva, resulting in changing reception of the vulva as target organ to hormonal stimulation.
The link between kraurosis and leukoplakia with impaired nervous system indicates functional changes in nerve endings, violation in nutrition of tissues, distinctive, often symmetrical arrangement of the lesions, the appearance of paraesthesia and persistent itching.
Restructuring of the neuroendocrine system in these patients is often accompanied by hidden and apparent violations of carbohydrate metabolism, hypertension, chronic liver disease, reduced thyroid activity. Age changes in the genitals are more pronounced than in healthy women. However, it is known that the syndrome of "exhaustion" of the ovaries (hot flushes to the head and upper body, excessive sweating, vaginal dryness, etc.) do not always lead to the development of kraurosis and leukoplakia. Apparently, they don’t cause much decline of ovarian function, but a change in receptor sensitivity of the vulva to hormonal factors. There are also indications of the role of vitamin deficiencies, especially vitamins A and E.
Clinic Picture (kraurosis /leukoplakia)
The disease begins silently in the milder forms not accompanied by any symptoms and is found only in prophylactic examinations. But often kraurosis is accompanied by itching of the vulva, mostly at night, paresthesia (numbness, crawling chills, burning sensation). Prolongeditchy feelingis often so excruciating that it leads to neurotic disorders (depression, increased irritability and even suicide attempts), deprives the patient of sleep and reduces the ability to work. The emergence of such a painful itching is due to violation of the trophic system tissue, growth of free nerve endings deprived of glial coverage and excessive action on them by proteases. Persistent itching leads to scratches, abrasions, tears and, ultimately, to inflammation of the vulva.
Diagnosis
In gathering medical history one record;the time of appearance of itch, its intensity, concomitant and prior itching disease, the efficacy of earlier treatment. Conduct a physical examination of the patient and investigation of smears on the flora of the cervical canal, vagina and urethra.
Differential diagnosis: There is need differentiate these background diseases with other pathological processes that have a similar clinical picture: lichen planus, candidiasis of the vulva, vitiligo, essential itching etc.
During a patient visit it is desirable to add colposcopy, which allows more accurate assessment of macroscopic changes caused by infection. During colposcopyexamination, mucosa looks from yellow to brick red in kraurosis. Sample taken is usually Schiller negative or weakly positive, suggesting the absence of glycogen in the cells of surface epithelium. On the whitish or yellowish surface they are clearly visible as a red mottle capillaries.
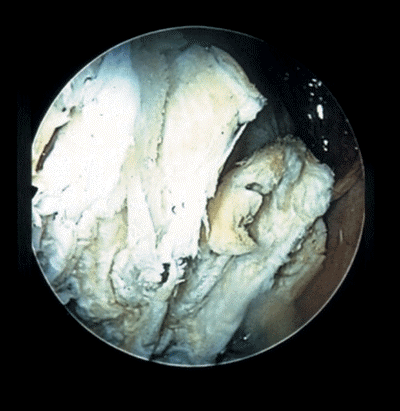
Colposcopy leukoplakia has a characteristic pattern of Keratinized opaque surface. Depending on its thickness, leukoplakia looks like a simple white spot, it forms a rough white surface due to lack of vessels. Often border leukoplakia has the form of geographical maps. Sample take is Schiller negative.
Treatment
Kraurosis and leukoplakia have a chronic prolonged course. Therefore therapy must be comprehensive, strictly personal and pathogenetically substantiated.
The patient should systematically follow the rules of personal hygiene. Washing of external genitalia should be carried out repeatedly during the day with boiled water, without soap, with the addition of baking soda, infusions of chamomile or marigold. Not recommended to use potassium permanganate, boric acid, as they dry and irritate skin tissues. Do not wear wool and synthetic underwear, as itching may increase.
One of the long-term methods of treatment is hormone therapy. The simultaneous use of estrogen and androgen hormones in order to reduce the stimulating effect on the endometrium and breast cancer is reccommended: an injection of estradiol dipropionate (0,5-1,0 ml 0,1% solution) and testosterone propionate (1 ml of 1% solution) in the same syringe in span of 5-7 days. Treatment is carried out for 5 to 7 weeks. Thereafter maintenance therapy follows. It involves, one injection of these hormones each month during the year. Androgens, which are less than estrogens, inhibit gonadotropic function of the pituitary, as well as significantly reduce the layers of inflammation relieving the itch.
Topical application of hormones in the form of ointments, creams, vaginal suppositoriesalso has a good effect i.e 0,1-1,5% testosterone cream, vaginal suppositories containing 0,5-1 mg diethylstilbestrol, 1 mg sinestrol, 5 mg of methyltestosterone. Course of treatment is 4-6 weeks.
Treatment can also be done using bio-stimulants: aloe extract to 1 ml daily (30 injections), ointment with 20 000 IU folliculin Linimentum and aloe. Course of treatment is repeated after 4-6 months, as the interval is gradually increased.
Local symptomatic therapy: a corticosteroid, prednisolon and others, with menthol and anestezin, with vitamin A.
Physiotherapy methods like use of ultrasound, which reduces the excitability of the autonomic nervous system, blocking an abnormal pulse,stimulating ovarian function and giving anti-inflammatory effect on tissues.
Pathogenetic therapy includes endonasal electrophoresis with vitamin B1 for the normalization of physical and chemical processes in the nerve cells of hydrocortisone phonophoresis in the area of the vulva, groin and perianal area (fibrinolytic, trophic, vazotropny effect), high doses of vitamin C, vitamin A to 1 ml / m 20 days.
Stubborn cases may be treated by alcohol-novocaine blockade and oxygen therapy. Alcohol-novocaine solution injected into the skin (ischiorectal space), blocks abnormal impulses, improves trophism and contributes to resorption plaques.
In recent years, cryotherapy (spray method), which prevents dangerous bleeding and the faster healing of wounds is used. It is painless, because under the influence of quick cooling destroys the sensitive nerve endings.
Vaginal intraepithelial neoplasia(VAIN)
Vaginal intraepithelial neoplasia(VAIN) is a condition that describespremalignanthistologicalfindings in thevaginacharacterized by dysplasticchanges.It is generallyasymptomatic.
The disorder is rare and may have no symptoms.VAIN can be detected by the presence of abnormal cells in aPapanicolaou test(Pap smear).
VAIN comes in three stages, VAIN 1, 2, and 3.
In VAIN 1, a third of the thickness of the cells in the vaginal skin are abnormal, while in VAIN 3, the full thickness is affected.VAIN 3 is also known ascarcinoma in-situ, or stage 0vaginal cancer.
Infection with certain, high-risk types of thehuman papillomavirusmay be associated with up to 80% of cases of VAIN.
One study found that most cases of VAIN were located in the upper third of the vagina, and were multifocal.In the same study, 65 and 10% patients with VAIN also hadcervical intraepithelial neoplasiaandvulvar intraepithelial neoplasia, respectively.
In another study, most cases of VAIN went into remission after a single treatment, but about 5% of the cases studied progressed into a more serious condition despite treatment.
Vulvar intraepithelial neoplasia
Vulvar intraepithelial neoplasia(VIN) denotes a squamous intraepitheliallesionof thevulvathat showsdysplasiawith varying degrees of atypia. The epithelialbasement membraneis intact and the lesion is thus not invasive but has invasive potential.
The terminology of VIN evolved over several decades. In 1989the Committee on Terminology,International Society for the Study of Vulvar Disease(ISSVD) replaced older terminology such as vulvardystrophy,Bowen's disease, and Kraurosis vulvae by a new classification system forEpithelial Vulvar Disease:
§Nonneoplastic epithelial disorders of vulva and mucosa:
§Lichen sclerosus
§Squamous hyperplasia
§Other dermatoses
§Mixed neoplastic and nonneoplastic disorders
§Intraepithelial neoplasia
§
§Squamous vulvar intraepithelial neoplasia (VIN)
§VIN I, mildest form
§VIN II, intermediate
§VIN III, most severe form includingcarcinoma in situof the vulva
§Non-squamous intraepithelial neoplasia
§Extramammary Paget's disease
§Tumors ofmelanocytes, non invasive
§Invasive disease (vulvar carcinoma)
Diagnosis
The patient may have no symptoms, or local symptomatology including itching, burning, and pain. The diagnosis is always based on a careful inspection and a targetedbiopsy.
Treatment
The treatment of VIN is local to wide excision, in case of very extensive involvement or recurrency even a simplevulvectomy. Laser therapy has also been useful for VIN.
Ectropion :
Cervical ectropion(orcervical erosion) is a condition in which the central columnnar epithelium protrudes out through theexternal osof thecervix.
There are two ways of ectopias:
1) at puberty with the increase of production of sex hormones ( "congenital pseudo");
2) after birth, with laceration of circular muscles is formed ectropion - eversion of the mucous cervical canal. During his lifetime, depending on hormonal status (menstrual cycle, pregnancy, menopause), changing shape of the cervix, and the boundary of the joint endo-and ectocervical is moved to the side of the cervical canal, the vaginal side of the (then formed by ectopia) . During menopause, most ectopias regresses.
Overlapping cylindrical epithelium layered flat epithelium is influenced by various exogenous and endogenous factors. There are two ways of overlapping ectopias:
1) due to metaplasia, ie, the transformation of reserve cells in a multilayer flat epithelium;
2) due to rise in the periphery of ectopia multilayer flat epithelium
Ectropion can be associated with excessive but non-purulentvaginal discharge due to the increased surface area ofcolumnar epithelium containing mucus-secreting glands. It may also give rise to post-coital bleeding as fine blood vessels present within the columnar epithelium are easily traumatized.
Cervical erosion is a normal phenomenon, especially in ovulatory phase on younger women,pregnantsand those taking the oral contraceptive pill which increases the body total estrogen level. It may be congenital problem by persistence of the squamocolumnar junction normally present in the intrauterine life.
Treatment
Usually no treatment is indicated for clinically asymptomatic cervical ectropions. Hormonal therapy may be indicated for symptomatic erosion. If it becomes troublesome to the patient, it can be treated by discontinuing the oral contraceptive pill, or by using ablation treatment under local anaesthetic. Ablation involves using a preheated probe (100 degrees celsius) to destroy 3-4mm of the epithelium. Observation and re-examination for 3 months after labour inpost-partumerosion.
Cervical Dysplasia
Cervical dysplasia is a cytological term to describe cells which resemble cells of carcinoma cervix. Cervical intra-epithelial neoplasia (CIN) refers to histopathological description where part or whole of thickness of cervical epithelium is replaced by cells showing varying degree of dysplasia.
Dysplasia
Represents a change casusing an alteration and disorderly arrangement of the cells of the stratified squamous epithelium.
3 classifications:
1.Mild dysplasia:
·(CIN-I) undifferentiated cells are confines to the lower third of epithelial layers. Cells are more differentiated towards the surface.
·Often seen in inflammatory disease like trichomoniasis.
2.Moderate dysplasia:
·(CIN-II) the lower 50-75% of epithelial layer is undifferentiated
3.Severe dysplasia
·Or carcinoma in situ (CIN-III) changes are similar and are considered a single entity. The entire thickness of epithelium is replaced by anaplastic cells. Stratification is lost. Basement membrane is intact and no stromal infiltration.
Symptoms and signs
Post-coital bleeding may be the only symptom. Cervicitis or erosion.
Diagnosis
·Cervical exfoliative cytology
·Speculoscopy
·Micro Colpohysteroscopy
·Colposcopy
·Cervicography
·Biopsies: punch biopsy, colposcopic directed biopsy, cone biopsy
Treatment
1.Local destructive methods
·Cryosurgery
·Fulguration/ coagulation
·Laser ablation
2.Excision of local tissue
·Conization by cold knife
·Laser conization
·LLETZ (large loop excision of the transformation zone)
3.Surgery
·Therapeutic conization
·Hysterectomy
·Hysterectomy with removal of vaginal cuffs
