Epistaxis- Nosebleeds- Bleeding from the Nose
- font size decrease font size increase font size
 Nosebleeds, also known as epistaxis, can be messy and even scary, but often look worse than they are. Many can be treated at home, but some do require medical care. When medical attention is needed, it is usually because of either the recurrent or severe nature of the problem.
Nosebleeds, also known as epistaxis, can be messy and even scary, but often look worse than they are. Many can be treated at home, but some do require medical care. When medical attention is needed, it is usually because of either the recurrent or severe nature of the problem.
What causes nosebleeds?
Epistaxis is extremely common. For unknown reasons, it most commonly occurs in the morning hours. Most do not have an easily identifiable cause. However, trauma is a very common cause as the nose is lined with many blood vessels that lie close to the surface.
Epistaxis can be divided into 2 categories, anterior bleeds and posterior bleeds, on the basis of the site where the bleeding originates.
- • Anterior haemorrhage - usually from the nasal septum, particularly Little's area which is where Kiesselbach's plexus forms (an anastomotic network of vessels on the anterior portion of the nasal septum).
- • Posterior haemorrhage - this emanates from deeper structures of the nose and occurs more commonly in older individuals. Nosebleeds from this area are usually more profuse and have a greater risk of airway compromise.
Conditions that predispose a person to nosebleeds include:
- • exposure to warm, dry air, such as in a heated home in the winter, for prolonged periods of time,
- • nasal and sinus infections, allergic rhinitis,
- • object stuck in the nose (foreign body)
- • vigorous/excessive nose blowing,
- • deviated or perforated nasal septum
- • Cocaine use. The drug is usually taken by inhalation and it has a very strong vaso-constrictive effect leading to sloughing and atrophy of septum.
- • Underlying disease process
-
- Liver disease, chronic alcohol abuse, kidney disease, platelet disorders, and inherited blood clotting disorders can also interfere with blood clotting and predispose to nosebleeds.
-
Vascular malformations in the nose and nasal tumors are rare causes of nosebleeds.
o Hereditary haemorrhagic telangiectasia (Osler-Rendu-Weber syndrome) causes recurrent epistaxis from nasal telangiectases.
o Juvenile angiofibroma is a highly vascular benign tumour that typically presents in adolescent males.
- • High blood pressure may contribute to bleeding, but it is often the anxiety associated with the nosebleed that leads to the elevation in blood pressure.
- • Certain medications
• aspirin, NSAIDs, warfarin, heparin, ticlopidine, and dipyridamole—not only predispose to epistaxis but make treatment more difficult.
• Topical nasal medications, corticosteroids and antihistamines, may sometimes lead to nosebleeds.
How are nosebleeds stopped?
Treatment depends on the clinical picture, the experience of the treating physician, and the availability of ancillary services. Treatments to be considered include topical vasoconstriction, chemical cautery, electrocautery, nasal packing (nasal tampon or gauze impregnated with petroleum jelly), posterior gauze packing, use of a balloon system (including a modified Foley catheter), and arterial ligation or embolization.
First aid - Self-Care at Home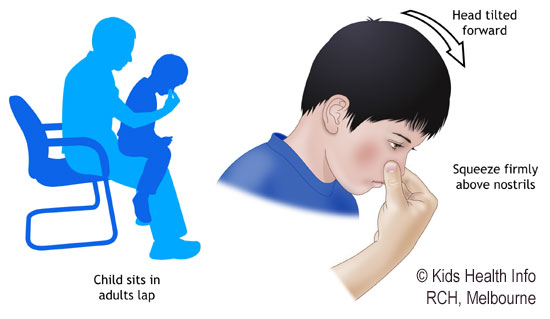
•Sit down and lean your body and your head slightly forward. This will keep the blood from running down your throat, which can cause nausea, vomiting, and diarrhea. (Do NOT Tilt your head back, lay flat or put your head between your legs.)
 • Use your thumb and index finger to pinch together the soft part of your nose. Make sure to pinch the soft part of the nose against the hard bony ridge that forms the bridge of the nose. Apply direct pressure for approximately 10 minutes. Time it to make sure the nostrils are not released earlier.
• Use your thumb and index finger to pinch together the soft part of your nose. Make sure to pinch the soft part of the nose against the hard bony ridge that forms the bridge of the nose. Apply direct pressure for approximately 10 minutes. Time it to make sure the nostrils are not released earlier.
• Spit out any blood in the mouth. Swallowing blood may make someone vomit.
This technique will stop the majority of simple nosebleeds. Once the bleeding has stopped, try to prevent any further irritation to the nose, such as sneezing, nose blowing, or straining for 24 hours. Nasal saline sprays or other lubricating ointments or gels also may be useful to promote tissue healing and keep the nasal passages moist.
When to Seek medical care
• Failure to stop the bleeding after more than 15 to 20 minutes of applying direct pressure.
• You experience repeated episodes of bleeding.
• The bleeding is rapid or the blood loss is large (exceeds a cupful).
• The bleeding was caused by an injury, such as a fall or other blow to the nose or face.
• You feel weak or faint/light-headed, that you are going to pass out;
• The blood goes down the back of your throat rather than out front through the nose even though you are sitting down with body and head leaning slightly forward, "posterior nosebleed," which almost always requires a physician’s care.
• You get a nosebleed that seems to have occurred with the start of a new medication.
• You get nosebleeds accompanied by unusual bruising all over your body and or additional bleeding from places other than the nose, such as in the urine or stool
• if you are taking any blood-thinning medications (for example, aspirin or warfarin [Coumadin]);
• if you have any underlying disease that may affect blood clotting, such as liver disease, kidney disease, or hemophilia
• if you recently had chemotherapy.
With proper treatment, the vast majority of people recover from nosebleeds with no long-term effects.
